
Over the counter medicine practice is common in Nepal (Pokharel S, Adhikari B. 2020)
Context
Nepal is one of the low- and middle-income countries that suffers from poor universal health coverage and a high burden of infectious diseases (Ranabhat et al., 2019; Mishra et al., 2015). Seeking health care at informal health sources such as at pharmacists and drug dispensers that can lead to buying antibiotics over the counter (OTC) is a common practice in Nepal (Raut and Adhikari, 2016; Raut et al., 2017). Drug shops serve to fulfil the limitations of poor health care infrastructure in developing countries such as Nepal; and thus, are an essential part of the health services (Sudhinaraset et al., 2013; Ranjit, 2016). Generic features of why patients buy antibiotics OTC include poor accessibility, costs, time, and low quality of services at formal health care centres. However, there are also specific reasons and mechanisms why such a practice occurs that are rooted in the local social and cultural context.
In order to explore socio-cultural drivers a qualitative study was conducted among patients, drug dispensers and clinicians between August to December 2019 in Eastern, Central, and Western Nepal (Figure 1). A total of eight Focus Group Discussions (FGDs) and five Semi-Structured Interviews (SSIs) were conducted among patients who were attending the tertiary hospitals. Four FGDs and eleven SSIs were conducted among clinicians and twelve SSIs were conducted among dispensers (BMJ Global Health, under review).
 Figure 1: Study sites on various provinces in Nepal.
Figure 1: Study sites on various provinces in Nepal.
The main findings of this study are summarized in Figure 2, which shows the complexity and number of interrelated factors of dispensing antibiotics in this Nepalese context.
Over the counter dispensing of antibiotics is a complex problem:
Facilitators of over-the-counter dispensing of antibiotics
Part of the reason why drug shops are popular in developing countries is due to their ease of accessibility and lower costs. While drug shops serve as informal health services, their quality, legitimacy and their competence can be questionable. Drug shops are often run by unqualified professionals and may provide sub-optimal care to patients (Ansari, 2019; Bhuvan, Alrasheedy, and Ibrahim, 2013). These limitations and disadvantages were in fact well-articulated to us by the clinicians and the dispensers themselves. They expressed concerns around the competence of (their) dispensers, and also questioned their legitimacy (e.g. using someone else’s licence).
Commercial incentives and lack of accountability
Drug dispensers in general may be less immersed in the clinical care when dispensing antibiotics to clients, offering services like a retail transaction. For instance, dispensers do not ask patients for follow-ups, since they may be driven by the economic incentives and lack adequate competence to deal with the poor outcomes. Rather, they typically instruct patients to visit doctors if their illnesses are not cured by the medicine provided. This practice seems to offer a safety net for dispensers to avoid accountability for any poor outcomes related to the medicines sold. At the same time, if these patients do get better, they would gain easy goodwill and return clientele.
Also, OTC visits at drug shops seem to be brief. Patients simply expect to get what they need in a short period of time. Many come with past medicine strips or blisters, old prescriptions, name of the medicines, and symptoms as hints to get the exact type of drugs that they were expecting rather than for clinical care. We found that a major incentive for patients was saving cost of visiting the hospitals, particularly related to medical assessments. Although visiting the drug shops at first sight does seem to save them cost, as patients can obviously appreciate that they do not have to spend money on investigations, they may buy unnecessarily expensive and advanced antibiotics.
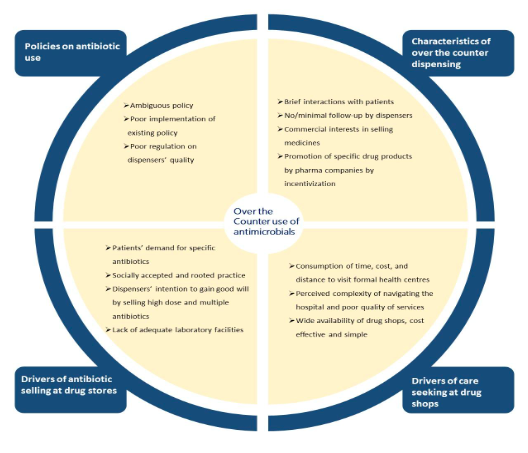 Figure 2: Summary of factors affecting OTC use of antimicrobials in Nepal.
Figure 2: Summary of factors affecting OTC use of antimicrobials in Nepal.
Easy loopholes in policies
Nepalese policies concerning the sale of antimicrobials, such as requirement of prescriptions and regulation, are not well developed. Although policy does seem to encourage cautious use of antibiotics (based on the judgement of a clinician), there were easy loopholes for drug dispensers to evade regulations in their practice. Drugs stores in Nepal are categorized to regulate its dispensing and prescription ability. Both category ‘A’ (Narcotics and poisonous drugs) and category ‘B’ (antimicrobials and hormones) can only be prescribed by a doctor and dispensed by a licenced pharmacist/professional. While category ‘A’ drugs need explicit records of their sell, category ‘B’ drugs do not require a record. So, in practice, specifically for category ‘B’ (antimicrobials), there is no need of prescription because they are not obliged to keep a record of the sales.
Low awareness of AMR among clients and patients
While the issue of OTC antibiotic dispensing is recognized to be a major problem due to its propensity to trigger resistance, antimicrobial resistance (AMR) was poorly understood by most of the patients in this study. Lack of knowledge about antibiotics and the meaning and consequences of AMR are major problems. Patients had no idea what ‘antibiotics’ were and while few made guesses, others perceived that they were highly potent medications (‘hard medicine’) against the diseases. Dispensers, while they were familiar with the antibiotics and was part of their routine sell, also could not provide details on how antimicrobial resistance developed. Only a few of them could make tangential explanation about antibiotics losing effectiveness due to AMR.
Points of discussion
Pedagogical notes
Acknowledgements
Sunil Pokharel, Shristi Raut, Janak Adhikari, Suman Thapa, Kumar Paudel, Narayan GC, Sandesh Neupane, Sanjeev Raj Neupane, Rakesh Yadav, Sirapa Shrestha, Komal Raj Rijal, Sujan Babu Marahatta, Phaik Yeong Cheah, and Christopher Pell.
Bipin Adhikari
Mahidol-Oxford Tropical Medicine Research Unit, Faculty of Tropical Medicine, Mahidol University, Bangkok, Thailand and Centre for Tropical Medicine and Global Health, Nuffield Department of Medicine University of Oxford, Oxford, United Kingdom.